Eczema is one of the most common skin conditions in children - affecting up to 25% of children at some point in their young lives.
This means a sizable portion of parents out there have to navigate and manage treatment options for their children. While most children will see fewer eczema flare-ups as they age, there is generally considered no “cure” for eczema itself.
So what does that mean for parents? It means that the treatments you select should be both effective and safe. It is critical to find a treatment, or range of treatments, that you feel comfortable using long-term with your children.
What is Eczema?
Eczema (also called atopic dermatitis) is a chronic, inflammatory skin condition. Symptoms can include dry or crusty patches, inflammation, and itchiness of the skin.
Those with eczema are not contagious and their symptoms are not the result of infection (though secondary infections can occur).
Eczema is a condition of the skin barrier. Eczema sufferers generally have a weaker skin barrier that allows irritants to pass through it more easily, which then leads to an immune response. This response can be magnified when the patient also has a more reactive immune system.
For reasons we will get into later, eczema tends to follow a cyclical pattern like the below:

We will walk you through the stages of eczema and the different contributing factors and then show you how you can use the available treatments to help your little one feel better.
What Are The Stages Of Eczema?
Eczema has a predictable cycle. Knowing this, it is easier to understand and interpret how treatment options can affect this cycle and which treatment is right for your child.
People with eczema tend to have an excess of short chain ceramides and not enough long chain ceramides in their skin. Long chain ceramides make up 50% of the skin barrier and a lack of long chain ceramides causes the skin barrier not to function well.

Figure 1: Too few long chain ceramides leads to a weak skin barrier
With a weakened skin barrier, it is easier for a skin irritant to passes through and kick off an immune response. If a person has an allergy, the allergen can act as a trigger as well.
The skin reacts to the irritant with an immune system response. The immune response can be amplified by an autoimmune disease or if the person has elevated levels of systemic inflammation. It is the immune response that leads to symptoms of dryness, rash, and crusty patches that tend to be itchy.

Figure 2: A weakened skin barrier allows irritants through to create an immune response
A weak skin barrier makes the symptoms of dryness and cracking worse as more moisture is able to escape a weak skin barrier.
After the immediate immune response there is a "resolution phase". This is where most of the symptoms are experienced. During resolution, the immune system is trying to figure out if the job is done.
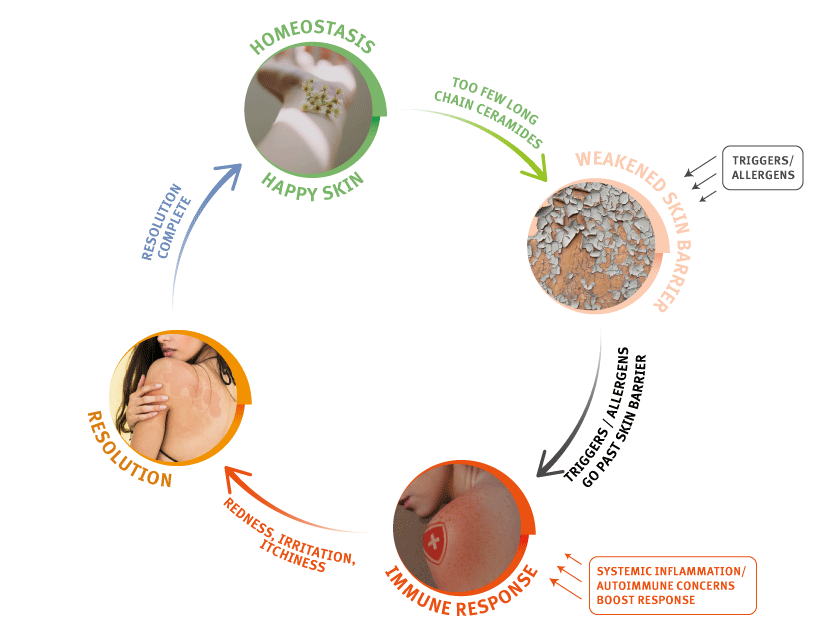
Figure 3. The complete eczema cycle from a weakened skin barrier back to homeostasis.
Eventually, the skin barrier is patched up, the immune response quieted, and the body returns to normal function, also called “homeostasis”.
In eczema patients, homeostasis is delayed because of the weakened barrier and possible immune system complications. New irritants, including those that are introduced through scratching or infection are able to pass through the barrier.

Figure 4. Complications such as scratching, infection, and excess short chain ceramides from the immune reaction can extend the eczema cycle.
Most eczema patients have a genetic disposition to a weakened skin barrier, and so they remain sensitive to new triggers, which can instigate a new eczema cycle.
The Relationship Between Eczema And Ceramides
Eczema is a result of a weakened skin barrier often characterized by a lack of long chain ceramides. Ceramides are the natural building blocks within your skin barrier. They work to protect your skin against irritants, seal in moisture and manage the inflammation response within the skin.
Long chain ceramides, specifically, act as a “glue” between the skin cells to form a dense and resilient skin barrier. Without enough of these, irritants can more easily trigger the tell-tale itching, rash and dryness that are the hallmark of eczema.
Even the healthy skin of eczema sufferers typically has fewer long chain ceramides than the healthy skin of an individual without eczema. The locations of eczema flare-ups have even fewer long chain ceramides.
If you want to learn more about the role of ceramides in a healthy skin barrier, you can check out our article here The Science of Ceramides In Skin Care.
Traditional Treatment Options
Looking at the eczema cycle, there are treatment options that attempt to address each component: triggers, immune response, resolution, and maintaining homeostasis. There are also treatments that address the various complicating factors like irritants, allergies, and systemic inflammation or autoimmune concerns.
Most often, by the time parents are speaking with a physician, they are in a full-blown immune response phase. The physician’s primary goal will be to address the immediate symptoms that pose a risk, such as itchiness, as persistent scratching presents an opportunity for new irritants to pass through the skin barrier and can cause a secondary infection.
Once the eczema flare symptoms have resolved, parents can work with their child’s pediatrician toward a long-term treatment plan to achieve less frequent flare-ups by addressing the underlying skin barrier and irritant issues.
Unfortunately finding the right treatment plan for eczema can be expensive and time consuming. Accessibility, cost, and practicality of finding long-term solutions are serious concerns.
The below is provided for educational purposes only, but we hope it shortens your time to find the right plan for your family. Rulo is happy to provide physician referral resources on request.
Let’s break down the most common types of treatments and what role they play in your child’s eczema:
Trigger Control

Children with eczema can greatly benefit from a proactive approach to decreasing triggers in their environment. Removing potential triggers, such as dust mites and other allergens and even irritants found in skin products or soaps and cleansers, reduces the risk of one penetrating the weakened skin barrier and instigating an eczema flare-up.
Here are some simple ways to minimize eczema triggers:
- Adding mattress covers to children’s bedding
- Frequent vacuuming to remove dust mites, pet dander and other allergens
- Opening windows to allow fresh air in and allergens out
- Use a HEPA filter in your home
- Avoiding smoke (tobacco, fireplace, grill)
-
Keeping skin clean, particularly for babies with eczema
*Pro-tip, if your baby suffers from eczema on their face, apply plain petroleum jelly around your baby’s mouth before they eat and/or nap to reduce the amount of saliva lingering on the skin, which can act as an irritant. - Minimizing skin irritants such as scented lotions and soaps, makeup, skin products that contain alcohol, etc.
- Lukewarm baths or showers
-
Avoid wool, synthetic fabrics or scratchy clothing (including zippers, velcro, etc.)
*Pro-tip, try to find natural fabrics such as 100% cotton, silk and bamboo which are more breathable materials that won’t trap sweat, germs and other irritants on your child’s skin -
Use moisturizing cream
*Pro-tip for infants and babies with eczema, create a habit of applying moisturizing cream at every diaper change - Aim for a moderate indoor climate - dry air can dry out the skin, and air that is too warm can cause sweating. Both of these lead to itching, which in turn allows irritants through the skin barrier.
-
Avoid unnecessary sun exposure and use sun protection. Sun exposure is drying to the skin, which can lead to itching and more irritants penetrating the skin barrier. It also induces increased short chain ceramides, which may block long chain ceramide production.
*Pro-tip, use a mineral sunscreen that is formulated for sensitive skin (or baby formulations) to reduce the risk of sunscreen acting as a trigger itself.
Immune Response Control

Once a flare-up has occurred, the goal is to reduce the symptoms related to itching, as that can allow additional triggers through the barrier or result in a secondary infection.
The immune system is generally responding in a healthy way to irritants, as a result many physicians will reduce symptoms with solutions we will cover in the Resolution Support section. However there can be complicating factors like an atypical immune response, where the immune system must be more directly addressed.
Suppression of the immune response comes with serious risks and potential side effects including new or worsening eczema flares. Because of this, doctors will generally recommend the least invasive solution and escalate as needed. Please speak with a physician about what is right in your case.
Local Anti-Inflammatory Treatments
Topical steroids
Topical steroids are creams that can be spread on the skin and contain a drug that suppresses immune response. A common example that you may find as an ingredient is hydrocortisone.
There are safety concerns with topical steroids, especially for younger children and children with darker complexions. Topical steroids risks include
- A rebound effect with more frequent flare-ups or even addiction. Steroids can thin the skin barrier, which can result in more frequent flare-ups unless steps are taken to repair the skin barrier
- Illness, irritation, and difficulty coping with stress. Studies have also shown that use of high-potency topical steroids can suppress the hypothalamic–pituitary–adrenal (HPA) axis in children.
- Discoloration of the skin. Those with darker complexions can experience discoloration and thinning of the dermis (the inner layer of skin) as quickly as within 7 days of use.
Using these on sensitive areas such as the face or genitals, or using too much or too high of a dose of the product, can lead to complications.
Topical steroids should ideally only be used at the direction of your pediatrician to ensure your child’s safety.
Colloidal Oatmeal Baths
This bathing method is used to calm inflammation and increase moisture retention. Colloidal oatmeal can be a powerful therapeutic for eczema sufferers for its role in supporting the skin microbiome and skin barrier function.
Baths are relatively safe, but with any bathing technique used for your child with eczema, it is important to remember:
- Water should not be too hot or it can cause excessive dryness and irritation
- Do not scrub or it can irritate and break the skin further
- Do not bath too frequently or it can dry out the skin further
It is critical to seal the skin with moisturizer immediately after the bath, after patting dry. Ideally moisturizing (or applying wraps) is done within 3-5 minutes.
Phototherapy
This is typically a treatment administered directly by a dermatologist, and involves the use of very narrow bandwidth ultraviolet light targeted on the affected skin. The UV light works to kill off immune cells in the skin (specifically mast and T cells), thereby reducing the inflammatory response. There are precautions that are recommended for patients seeking phototherapy treatment - including avoiding sunlight and additional sun protective care.
Phototherapy itself is more practical for older children who can cooperate with the process, and is focused on more moderate to severe cases of eczema that is resistant to other treatment methods.
It is considered safe, but with UV radiation in general, there are side effects including dry skin, sunburn-like skin irritations, premature aging of the skin and risk of cancer.
This is not considered a long-term cure for eczema, and can even be a source of further eczema flare-ups due to the drying out and weakening of the skin barrier from the therapy.
Systemic Anti-Inflammatory Treatments
Increased overall inflammation in the body may lead to a stronger immune response to the irritants that penetrate the skin barrier. Reducing inflammation throughout can allow the body to respond more gently when presented with a trigger.
Antihistamines
These are medications that treat allergic reactions within the body, and they are used in children with eczema to treat pain and itching. Common examples are Benadryl, Zyrtec and Atarax.
There are a number of studies concerning the safety of antihistamines in children. They are widely known to cause drowsiness, and can also impair the child’s gross motor skills and cognition.
Diet
Participating in an anti-inflammatory diet - especially reducing the consumption of processed and fried food - can help to calm the body’s overall inflammatory response, and in the long-term, return the body’s natural immune defense system to a more neutral state.
Other Systemic Treatments
There are other medication therapies, all of which require prescription due to the potential significant side effects and interactions. They should be used only at the discretion of your pediatrician to ensure safety and proper dosing. These can include:
- Systemic immunosuppressants
- Topical calcineurin and/or PDE inhibitors
- Oral steroids
Resolution Support

The body must signal that the immune response is no longer needed in the resolution phase, but the resolution phase is also the phase where most symptoms are experienced. As a result, it can be easy to get trapped in a flare-up cycle where skin is dry and cracks or is scratched and new irritants or infections pass the skin barrier to kick off additional immune responses.
There are a number of treatments to help reduce the symptoms and chances of new irritants passing the skin barrier so that the body can quiet the inflammatory response and return to normal function.
Emollients
These are creams that aim to seal in moisture to the skin and protect the skin from further irritants. This allows the skin barrier to heal and therefore calm the immune response. Common examples of emollients include Vaseline, Aquaphor, Cetaphil, Eucerin and many others. Emollients are generally considered safe with few side effects. They are recommended in all pediatric cases of eczema, due to their safety and they can even help reduce the need for topical steroids.
Our Calming Serum works as an emollient, with the added benefit of inducing long chain ceramides on the skin barrier and supporting the microbiome reducing dry, red, itchy skin. Long chain ceramides can help rebuild the skin barrier to prevent more eczema flare-ups.
Wet/dry wraps
Another way to seal in moisture and calm the immune response, this entails the use of an emollient directly on the skin, followed by a layer of wet bandage, and then a layer of dry bandage. The wrap/bandage works to seal in the emollient to the skin and avoid drying of the skin. It also helps to improve itching.
Vitamin B12 cream
This has been shown to help reduce the extent and longevity of an eczema flare-up. This is achieved through lowering the levels of free nitric oxide in the skin, which results in less itching and therefore the skin barrier can heal faster. There have not been any major studies on the side effects or safety concerns of vitamin B12 applied topically.
Antibiotics (Complementary Treatment)
The weakened skin barrier in eczema patients provides an environment for “bad bugs” to thrive. The bad bugs look like irritants to the body or they allow irritants through the skin barrier. In both cases, they delay resolution of the flare-up.
Scratching of the skin can also create a secondary infection that may be serious.
To combat the bad bugs and/or infection, your doctor may prescribe antibiotics to reduce the bacteria.
With all antibiotics, common side effects include nausea, stomach pain, diarrhea. And, importantly, antibiotics disrupt the microbiome (the healthy bacteria that live within our body) which can lead to more inflammation and higher risk of infection.
Bleach Baths and Baking Soda Baths
These bathing methods can be effective in targeting the bacteria on the skin. Patients with eczema have been found to possess a higher concentration of Staph aureus bacteria on the skin, which can contribute to infection during an eczema flare-up. It is noteworthy that while bleach baths are a common recommended at-home treatment for eczema, there are studies that question the overall efficacy of bleach baths to reduce Staph aureus compared to plain water baths.
Bleach baths must be prepared with strict measurements, so as not to cause irritation to the skin. Bleach can be very drying if used improperly which can further exacerbate eczema symptoms. It can also be a severe irritant if bleach gets into the eyes, nose or mouth.
Baking soda can also, in some cases, lead to an imbalance of the skin pH and if used improperly can even lead to metabolic alkalosis.
Antimicrobials, like bleach and baking soda, not only wipe out the “bad bugs” on the skin, they also destroy the “good bugs” that comprise a healthy skin microbiome. A balanced skin microbiome supports the healthy functioning of the skin barrier and therefore reduces the likelihood of an eczema flare-up.
Antivirals (Complementary Treatment)
Antivirals are not a direct treatment to eczema. They are used to treat a viral infection that may occur alongside eczema called “eczema herpeticum” (eczema with herpes infection), which requires urgent evaluation and treatment with antiviral medications. If the eye area is affected, it can lead to blindness. The virus can also spread throughout the body if left untreated.
While antivirals are critical for those with eczema herpeticum, there are side effects to be aware of which can include nausea, diarrhea, dizziness. More severe side effects of antiviral drugs in children have been documented to impact the nervous system in a wide range of symptoms.
Homeostasis Support

When the skin barrier returns to “normal” and the immune response quieted, the skin will return to its normal function. There are treatments that can help maintain this stability and lessen the likelihood of a future flare-up. However, because eczema patients have a genetic disposition to producing too few long chain ceramides in their skin barrier, they will remain sensitive to new triggers, which can instigate a new eczema cycle.
Barrier maintenance
The root of eczema is a weak skin barrier. To repair and strengthen the skin barrier, you can:
- Ensure consistent use of emollients
- Seek skincare products that are targeted to adding long chain ceramides to the skin barrier
- Avoid application of products and/or treatments that disturb the balance of the skin microbiome
Reducing stress and/or anxiety
Taking steps to help your child manage stress and anxiety can help shield their body from chronic inflammation. Meditation, deep breathing, yoga and journaling can act as therapeutic aids and calm the body’s reactivity to triggers.
Stopping The Eczema Cycle With Barrier Strengthening
Eczema starts (and continues) with a trigger passing the skin barrier.
But you may have noticed a problem in the eczema cycle diagram we have been referring to: once you are in flare-up, it becomes easier to stay there. We call this "The Eczema Trap".

Scratching can cause new triggers to get through the barrier.
Infection can cause an additional immune response and the resultant symptoms.
But most dangerous of all: the immune response weakens the skin barrier and triggers that were previously rejected by the skin barrier pass through and you are locked into an eczema flare long-term.
Strengthening the skin barrier can break this cycle and lower the chance of a flare-up in the first place.
Long chain ceramides make up 50% of the skin barrier and are responsible for much of its function. Eczema sufferers tend to have fewer long chain ceramides in their skin and there is evidence that this lack of long chain ceramides is the root of eczema itself.
We recommend finding a skincare product with long chain ceramides as part of restoring and keeping your skin barrier strong.
Please consider our Calming Serum as part of your search. It induces long chain ceramides on the skin barrier and feeds your microbiome (which also helps reject triggers).
References
We are a team of scientists and physicians who deeply research to bring you the latest accurate information. Wherever possible we cite 3rd party research that is not backed by industry labs. Below are the papers we used to bring you this article.
The Science of Ceramides in Skin Care
Ceramides And UV/Radiation Exposure
Childhood atopic dermatitis: current developments, treatment approaches, and future expectations
Bathing, Moisturizing and Wet Wraps
Phototherapy with Narrowband UVB
Management of Severe Atopic Dermatitis in Pediatric Patients
Eczema: Light therapy and oral medications
Defending Against Disease with an Anti-Inflammation Lifestyle
Safety of antihistamines in children
Childhood atopic dermatitis: current developments, treatment approaches, and future expectations
Eczema bleach bath: Can it improve my symptoms?
Bathing, Moisturizing and Wet Wraps
SHOULD I ADD ANYTHING TO THE BATH OF A CHILD WHO HAS ECZEMA?
Bleach Bath Recipe for Skin Conditions
Metabolic alkalosis secondary to baking soda treatment of a diaper rash
Pediatric Atopic Dermatitis: A Review of the Medical Management
Childhood atopic dermatitis: current developments, treatment approaches, and future expectations
Evaluation of topical vitamin B(12) for the treatment of childhood eczema
Neuropsychiatric Effects of Antiviral Drugs
Write on: the healing effects of sharing your eczema journey
About The Author
Dr. Nicole Scott, PhD, MPH has published 29 peer-reviewed papers regarding human biology and the microbiome. Her work has been cited over 4000 times.
She is the Founder of Cybele Microbiome and Rulo Skin.